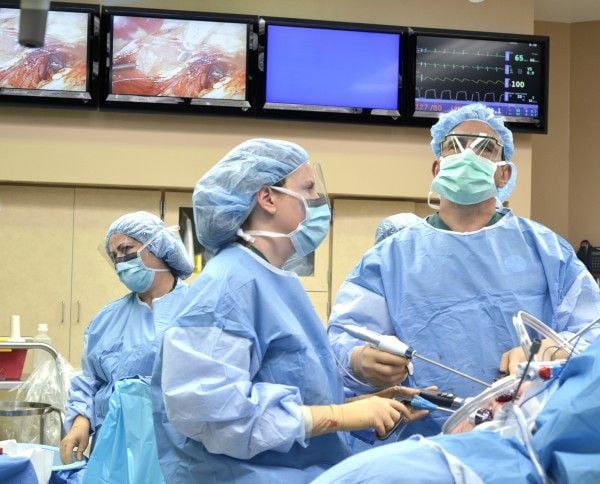
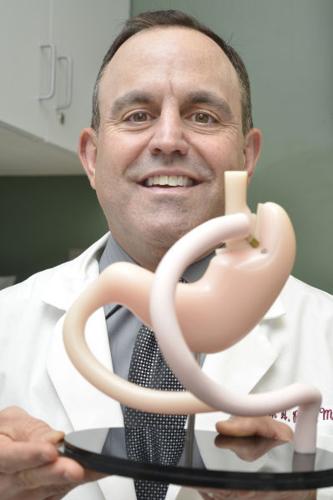
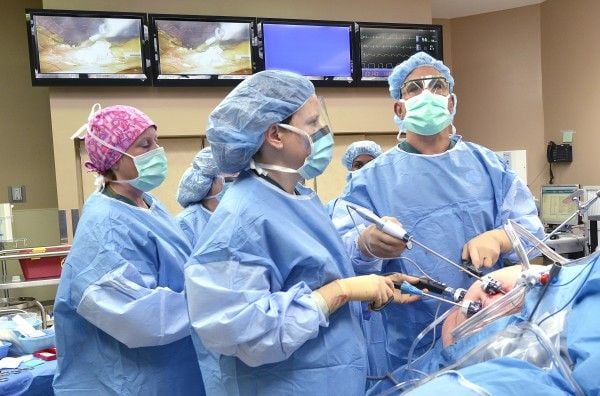
William Rizk said he might surgically remove a patient's gallbladder the day after he or she first visited his office at Midland's Clinic in Dakota Dunes. Getting into the operating room for weight loss surgery, he said, won't be as quick.
Bariatric surgery is a last resort for obese patients who have struggled to lose weight for years through diet and exercise. It's a process that requires medical, dietary and behavioral education in addition to significant lifestyle changes on the part of the patient.
"You have to know how you're going to live with this complicated tool," Rizk said. "Patients want their surgery and they want it now. But after patients go through surgery, many times they will remark that it was definitely worth their time and it did help them to be less anxious and more compliant after surgery."
The number of Siouxlanders going under the knife to slim down is growing as the obesity epidemic is getting worse.
People are also reading…
The American Society for Metabolic & Bariatric Surgery estimates that 158,000 bariatric procedures were performed in the United States in 2011. The number increased by 21,000 in 2013.
Last year, Rizk and his colleague, Dr. Keith Vollstedt, performed 112 bariatric surgeries, up from 2013.
Rizk attributes this recent rise to the laparoscopic sleeve gastrectomy, a procedure that debuted in May 2013.
People between the ages of 18 and 65 are candidates for weight loss surgery. Their body mass index -- the relationship between height and weight -- must be 40 or greater. A patient with a BMI of 35 could be considered, according to Rizk, if they have a medical problem related to obesity such as diabetes, high blood pressure, high cholesterol, sleep apnea, heart disease or chronic heartburn.
Before insurance companies will consider covering weight loss surgery, Rizk said, patients must show they've tried at least 10 different diets to lose the weight and failed. They are required to attend an obesity seminar at Midlands Clinic to educate themselves about options, participate in a support group, and undergo a psychiatric evaluation.
On average, Rizk said, two to three months passes from the first time patients walk into the clinic to the date of surgeries.
"The patient makes a selection based on what they feel is the most appropriate for them. We'll match that decision with what we feel is the best surgery medically for them," he said. "We'll incorporate their choice. We'll incorporate their BMI number. For example, if the patient has an extremely high BMI, we may err toward the side of our most effective surgery which is the gastric bypass."
PICKING THE RIGHT PROCEDURE
Laparoscopic gastric banding, largely due to consumer marketing, Rizk said, brings people to Midlands Clinic because they believe the surgery is safe and effective.
The procedure consists of placing a band around the upper part of the stomach to create a small pouch to hold food.
"Lap band gets people in the door because they think it's easy, but then when they learn about it, they sort of realize that gastric bypass and sleeve gastrectomy are dramatically more effective and carry just a slight increase in risk," he said.
Laparoscopic gastric bypass, Rizk explained, is the best approach to combat diabetes because of the way it causes food to digest and the hormonal changes it brings about. It divides the stomach into a small upper section, where food will go when eaten, and a larger bottom section. The small intestine is rearranged to connect to both sections.
"Bypass is a little more popular nationally, but sleeve has really picked up momentum over the past few years and is really becoming a very popular choice for weight loss surgery," he said.
Laparoscopic sleeve gastrectomy, the newest weight loss procedure, ranks virtually neck and neck with laparoscopic gastric bypass. A portion of the stomach is removed in laparoscopic sleeve gastrectomy and the remaining stomach is reshaped into a sleeve.
Last year, Rizk and Vollstedt performed six bands, 51 sleeves and 55 bypasses.
With any surgery, there are risks. But Rizk said weight loss surgery has become much safer over the past decade with advances in laparoscopic techniques.
In rare instances after laparoscopic sleeve gastrectomy and gastric bypass, he said food and drink may leak into patients' abdominal cavities. There are drawbacks to the sleeve too. The procedure can actually cause about 10 to 15 percent of people who have it to develop heartburn that can only be managed with medication.
"If someone would come in with heartburn, and they're really interested in a sleeve, it doesn't exclude them from the surgery," Rizk said. "But we would counsel them that it's very likely you would not get off this medicine."
THREE SMALLER MEALS KEY
Patients who opt for laparoscopic sleeve gastrectomy or gastric bypass can expect to lose weight over a one-year period.
The majority of their weight, Rizk said, will be shed in the first six months.
Weight loss with laparoscopic gastric banding is a slower process that takes about two years.
"With band weight loss it's much less predictable," Rizk said. "It's more difficult to obtain an excellent result."
For two to six weeks, depending on which surgery the patient had, they will eat a liquid diet of soup and cream of wheat, before moving onto pureed foods, soft foods and a regular diet.
"All weight loss surgeries take you from eating a big meal to eating a dramatically smaller meal but not feeling hungry," he said. "Through our education we teach that you just eat three meals after surgery."
No matter what procedure a patient has, gaining the weight back is a real possibility, Rizk said, if they "graze" or eat multiple small meals throughout the day.
"In the surgeries that we offer now, almost never does it come down to patients stretching out their stomachs. That is a misconception in my opinion," he said. "Ninety-nine point nine percent of the time people who gain their weight back are grazing."